For many years now, different obesity surgery procedures applied to the intestine or stomach have been done in order to boost weight loss. Losing weight is beneficial for people who have type 2 diabetes since in that way they have better control over their condition.
According to medical research, obesity surgery might directly impact the way the body uses the hormone insulin.
Not only does this surgery improve the blood glucose levels and helps lose weight, but it helps people to have better management of type 2 diabetes.
Here’s How:
- It improves the way the cells use the hormone insulin, and that leads to lower blood glucose levels;
- It changes the way the hormones present in the gut work and that, on the other hand, impacts the way the body uses this hormone;
- This surgery increases the number of bile acids which the body produces. The acids contribute for the cells to become more sensitive to the hormone insulin.
Different Forms of Type 2 Diabetes Surgery
There is a modified version of type 2 diabetes surgery, also known by the name bariatric surgery.
The options for surgery are the removal of a specific part of the stomach in order to lower the size of the stomach and in that way restrict the food intake and appetite. Or another alternative is a re-route of the digestive system in order to bypass the stomach.
Both treatments actually help individuals to lower their intake of food since they will feel full with less food. Also, that can benefit the way; their body uses the hormone insulin.
When the surgery is performed with the purpose to manage diabetes, the weight-loss or bariatric sugary is known the name “metabolic surgery.”
This also stands for Roux-en-Y “gastric bypass” surgeries that lower the size of the stomach to a small pouch. Then they plug it in the middle of the small intestine.
Also, it includes “sleeve gastrectomy.” In this procedure, the deep part of the stomach is removed, and the rest of the stomach is stapled together in shape similar to the sleeve.
Putting a band around the stomach with the purpose to shrink the stomach, gastric banding, is also thought to be a metabolic sugary.
Who Can Have Such Medical Procedure?
According to NICE obesity guidelines, this weight loss surgery is recommended for those people who meet specific strict criteria; this includes those people who recently got their type 2 diabetes diagnosis.
But, usually, surgery is offered for a restricted group of individuals who have gone through suitable lifestyle changes or have got medical treatment for weight loss.
But guidelines of NICE for type 2 diabetes don’t recognize sugary as a treatment options people who have type 2 diabetes.
New Guidelines on Surgery for Type 2 Diabetes
In May 2016, a group of international diabetes organizations, such as Diabetes UK and other 45 organizations, published new international guidelines on sugary for people with type 2 diabetes.
According to this group, obesity sugary, that was at first made to boost weight loss, needs to be included in the current option for treatment when it comes to specific categories of individuals who have type 2 diabetes.
Based on these new guidelines sugary needs to be recommended in case people:
- Have a Body Mass index, i.e., BMI over 40, no matter of how well they manage their condition or what other treatments they’re undergoing;
- Have body mass index from 35 to 20 with blood glucose levels which aren’t sufficiently controlled by taking drugs or following a healthy lifestyle;
- Have type 2 diabetes, body mass index from 30 to 35 and their blood glucose levels aren’t well managed by taking drugs or following a healthy lifestyle.
Risk of Diabetes Surgery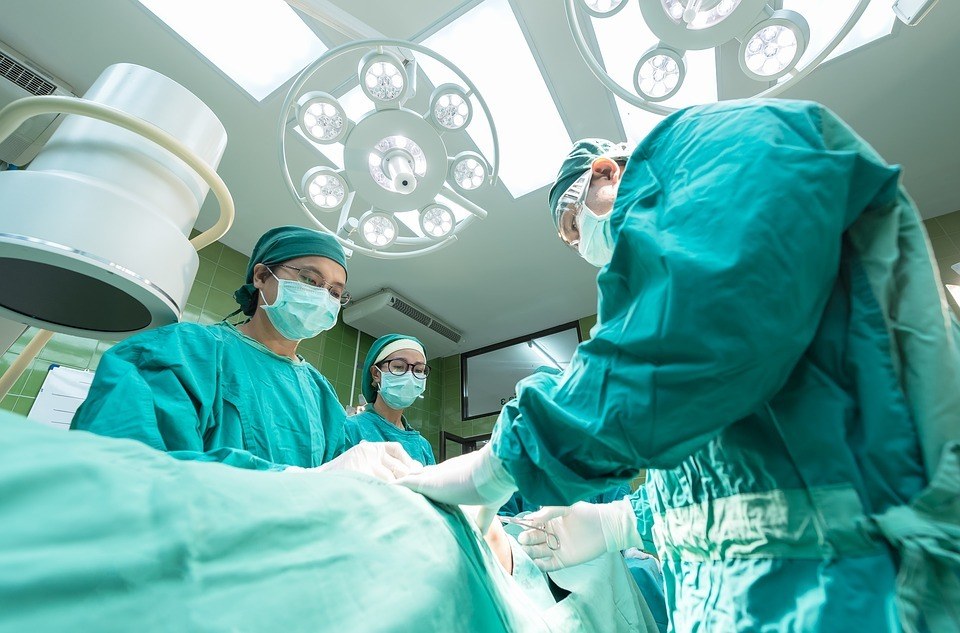
People probably wonder whether there are any risks from this surgery. Well, bear in mind that all surgeries come with a small element of risk.
However, when it comes to sugary for type 2 diabetes, this surgery doesn’t have any bigger risk than the standard surgical procedures.
But, in the long term, there might be a small risk of nutritional deficiencies like the need to take nutritional supplements or vitamins and anemia. In addition, there might be a need for regular monitoring and consultation.
The director of Health Intelligence and Professional Liaison at Diabetes UK, Simon O’Neil talks on this topic.
According to O’Neil, they support the call for surgery to be recognized as a treatment for type 2 diabetes, of course, alongside treatments like drugs to lower blood sugar and following a healthy lifestyle.

