According to the National Eye Institute, diabetic retinopathy is the number one cause of blindness in US adults, and the most common diabetes-related ocular disease. This eye disease affects people who have diabetes for a long time.
What’s concerning is that it usually shows no symptoms in the early stages, so it may progress significantly before you realize you have it.
If left untreated for a long time, it can lead to blindness and other eye problems.
What is Diabetic Retinopathy Exactly
It’s an eye disease that affects people with diabetics who have poor blood sugar control. It happens when changes in blood sugar levels lead to changes in the blood vessels in the retina. Sometimes, these blood vessels can swell up and allow fluid leakage into the rear of the eye.
But, abnormal blood vessels can also appear on the retinal surface area. If not treated on time, this eye disease can gradually worsen and cause many vision problems, including blindness. There are three types of diabetic retinopathy:
- Background retinopathy – early stage;
- Diabetic maculopathy – macular damage;
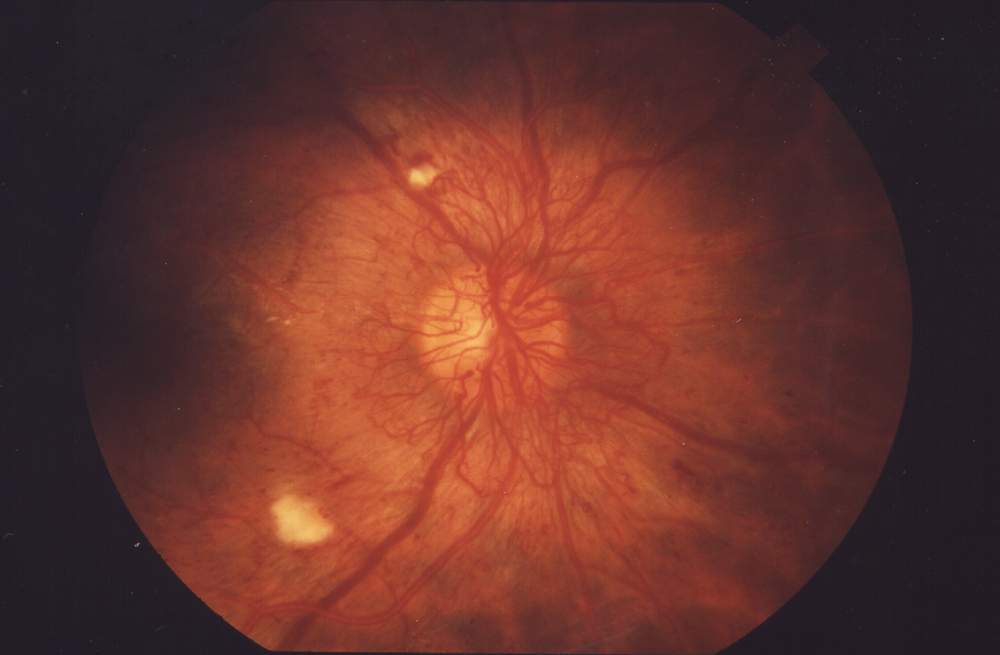
- Proliferative retinopathy – retinal damage, scarring, often leading to blindness (shown in the image below).
Symptoms of Diabetic Retinopathy
Even though early stages of diabetic retinopathy come with no symptoms, over time you could notice the following changes:
- Blurred vision;
- Spots or eye floaters;
- Impaired color vision;
- Fluctuating vision;
- Vision loss;
- Empty or dark areas in your vision.
Causes of Diabetic Retinopathy
Constant high blood sugar levels can lead to diabetic retinopathy. The high blood sugar levels can gradually weaken and damage the retinal blood vessels, thus causing swelling, exudates, and hemorrhages.
This, in turn, deprives the retina of oxygen, leading to a formation of abnormal vessels. That’s why proper blood sugar control is crucial for the prevention and treatment of this diabetes-related eye condition.
What’s more, those in an advanced stage of diabetic retinopathy could also suffer from glaucoma due to eye nerve damage.
Risk Factors
Anyone with diabetes is at risk of many eye problems, including cataracts, glaucoma, and diabetic retinopathy. Their risk increases with the following risk factors:
- Protein in urine;
- Poor blood sugar control;
- Hypertension;
- Increased triglycerides (fats) in the blood;
- Prolonged diabetes.
How to Treat It
The best way to prevent this eye disease from progressing is to control your blood sugar levels. This will prevent optic nerve damage and lower the need for laser surgery to prevent vision loss in future.
But, controlling blood pressure and cholesterol levels will also lower the risk of eye problems.
In case these methods don’t work for you, the next step is laser surgery. This medical procedure will help you reduce the swelling in the retina and slow the ocular fluid leakage.
In addition, there are specific drugs which can help reduce the leakage of fluid into the eyes and improve eye health.
How to Prevent It
Generally, all people with diabetes could develop this eye disease. But, even though you can’t fully prevent it, you can at least do something to reduce the risk. Take the following measures to help reduce the risk of diabetic retinopathy:
- Proper diabetes management – exercise, diet, and other lifestyle changes;
- Taking an annual dilated eye examination;
- Check your hemoglobin;
- Monitoring blood glucose levels;
- Control your blood pressure and cholesterol levels;
- Pay more attention to changes in your vision;
- Quit smoking.
Note – rapid improvement in blood sugar levels in people with diabetes can worsen diabetic retinopathy (30 mmol/mol drop in HbA1c.) So, if you have high blood glucose levels, try to reduce them gradually.