Diabetes mellitus i.e. diabetes actually portrays a group of specific diseases in which usually individual experiences high blood sugar, also known as blood glucose.
It is like that either to incomplete insulin production, the incorrect response of the cells to insulin, or maybe both. To be more specific, diabetes is actually a long-term condition that leads to high blood glucose levels.
But diabetes is not something that appeared recently. The first records of diabetes go even 2,000 years back. Although at that time often misunderstood, this condition has been identified as a deadly and devastating disease for more than 2,000 years.
Read on to find out more about the marvelous journey of medical advances and scientific discovery.
1552 B.C.
The physician Hesy-Ra wrote the first known record of this condition on Third Dynasty Egyptian papyrus.
This physician mentions the frequent urination, i.e., polyuria as a symptom. Also, around that time, the ancient healers noted that the ants are attracted to the urine of those who had this condition.
First Century A.D.
Arateus, the Greek physician, portrays the condition as “ the melting down of limbs and flesh” into the urine. In the first century, Aretaeus portrays the destructive nature of the condition naming it “diabetes.” Diabetes is a Greek word for “siphon.”
This Greek physician-prescribed his patients’ gruel, dates, oil of roses, and raw quinces. Other doctors prescribed fresh flowers of blind nettles, gelly of viper’s flesh, sweet almonds, and broken red coral.
164 A.D.
Galen of Pergamum a Greek physician mistakenly diagnoses diabetes as a condition of the kidneys.
Up to the 11th Century
Believe it or not, but diabetes was diagnosed by “water tasters”. “Water tasters” were people who drank the urine of those suspected of diabetes. The “water tasters” usually said that the urine was sweet-tasting.
And as a matter of fact, the Latin word for honey “Mellitus” was added to the term diabetes. That is how this condition got its name.
16th Century
Paracelsus around this time identified diabetes as a severe general disorder. And as the doctors learned more about the condition, they began to understand that diabetes could be managed.
That lead to the first diabetes treatment – prescribed exercise, usually horseback riding. The doctors thought that exercise would help relieve the frequent urination.
1700s & 1800s
Doctors began to realize that dietary changes might help in the management of diabetes. That is why the patients were usually advised to eat only the meat and fat of the animals.
Priory, the French physician, oddly advised his patients to consume large quantities of sugar.
The 1870s
Apollinaire Bouchardat, a French physician, in time of the Franco-Prussian War in the early 1870s, observed that there was an improvement in the symptoms of the diabetes patients. This was because of the food rationing related to war.
He started to make individualized diets as a treatment for the condition. This caused different fad diets to appear in the early 1900s. Some of these fad diets were the “starvation diet”, “oat-cure” and “potato therapy”.
Early 19th Century
The creation of the first chemical test in order to measure and indicate the presence of sugar found in urine.
Late 19th Century
Catoni, the Italian specialist for diabetes, isolated his patients just to follow the diets. Believe it or not, but kids were given cardboard or a hat box as a birthday cake in order to stimulate the blowing of the candles.
In that time, most of those who had diabetes were expected to live only 1 year after their first diagnosis.
1920 Dr. Best and Dr. Banting – Insulin Development
A scientist in Ontario, Canada, Frederick Banting studied the dynamics of diabetes. Banting together with his partner, Charles Best, had the idea to use insulin in order to treat diabetes.
He tested this theory in animal tests. He removed a pancreas of a dog, and then he injected it with extracted pancreatic islets.
Best and Banting managed to keep the dog alive during the whole summer just by administering insulin. And the results were regulation of the blood glucose levels.
Insulin Trials
The man, Professor J. MacLeod, the one who had given Best and Banting use of the university laboratory was impressed with the trial. He wanted further tests to be done.
After another successful trial, this professor made his whole research team work on only one goal, the purification, and production of insulin.
The team consisted of MacLeod, Banting, Collip, and Best. They worked together in order to make enough pure insulin to run a human trial. The final results were glorious.
Awakening from Keto – Acidosis
The researchers went to a hospital ward with children with diabetes. Most of the children were in a coma and were dying from diabetic ketoacidosis.
This specific moment is one of medicine’s most spectacular moments. There was a room full of parents who were sitting at the bedside waiting for the inevitable death of their kid.
The researchers went from bed-to-bed, and they injected the kids with insulin, the new purified extract.
As they injected the last child, the first one began to awaken from a diabetic coma. Then amazingly one by one, all kids awoke from the comas. Then the room of gloom and death became the place of hope and joy.
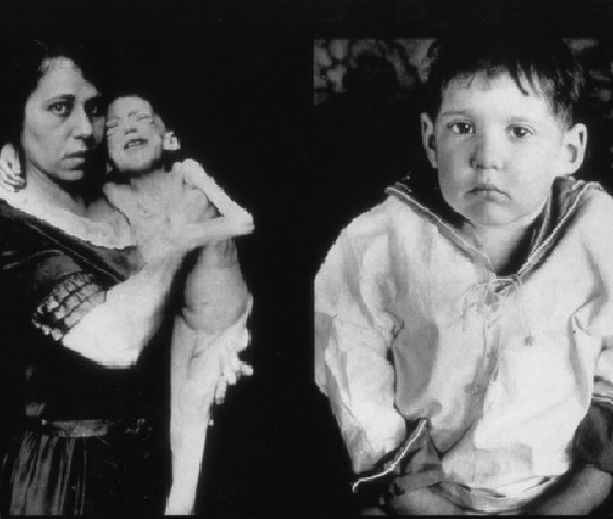
Life Before and After Insulin
Although there were many nutritional and medical efforts before the discovery of insulin, this condition led to premature death. In the photo, you will see a kid before insulin therapy and after insulin therapy.
Elli Lilly Company
Banting and Best continued to try and improve the extract. As a matter of fact, they could make enough for the demand of the hospital. Their work was actually only privately published.
However, the Eli Lilly Company understood this success and offered to be part of the project. In no time this company was making big quantities of refined pure insulin.
The insulin patent was sold to the University of Toronto for 1 dollar. And in that time 1 dollar was around $11.50 today.
Nobel Laureates
In 1923 MacLeod and Banting (right) were awarded the Nobel Prize in Physiology for Medicine. MacLeod shared his award with Collip, and Banting shared the award with Best (left).
Moreover, the co-inventor of insulin, Dr. Frederick Banting on June 3, 1934, was knighted for this medical discovery.
First Insulin Pump
The picture below is actually among the first prototypes of an insulin pump. This was an insulin pump in the late 60s. The insulin pump had a giant backpack and tubing inserted, and it was similar to an IV.
Furthermore, home glucose testing units were made available during the 60s.
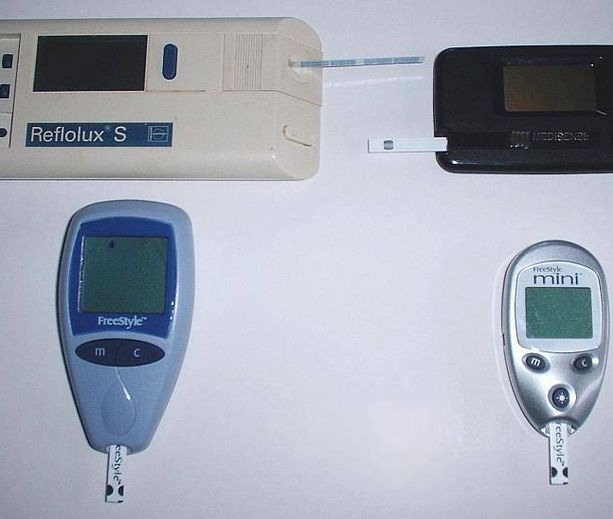
The Evolution of the Blood Sugar Meters
The first blood glucose meters were sometimes inaccurate and bulky. Also, they needed a significant amount of blood. But over the years, they are more accurate and smaller. And they only need a pin drop of blood.
1986
The first insulin pen was introduced in 1986. This step made insulin delivery much more mobile for all people who take insulin to school and work.
The Pump Technology
Insulin pumps deliver short or rapid-acting insulin 24/7 through a catheter that is placed under the skin.
The insulin has 3 types of doses: basal rates for a small dose of insulin during the day and night, then bolus doses to cover carbs in meals, and last but not least supplemental or correction doses.
The latest pumps work together with continuous sugar monitoring which will alarm in case the blood glucose is too low or too high.
Diabetes Support Tools
There are many options for those with diabetes to use social networks that empower these people. Apps and websites for smartphone simplify the way to share treatments, start conversations, post and read product recommendations, etc.
Diabetic Connect’s app involves a blood glucose log and offers a format to link with others who have diabetes.
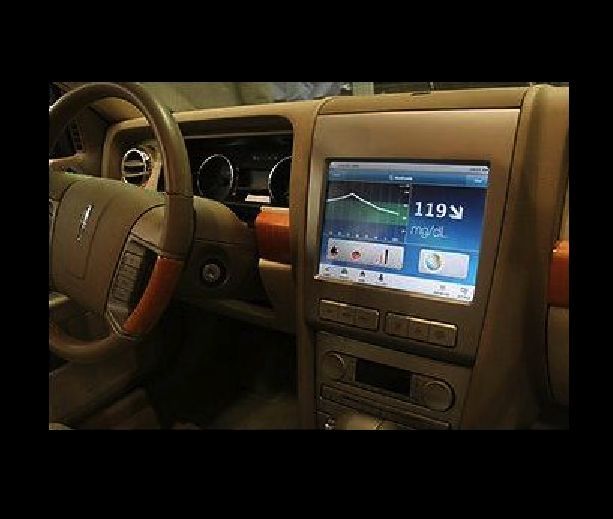
A Car Which Will Tell the Blood Glucose Level?
Yes, this is possible. Medtronic has made a dashboard-mounted device that works side by side with a continuous sugar monitor in order to track the blood glucose levels of the driver.
The monitor uses a wireless sensor that samples the blood sugar level of the driver every couple of minutes. Moreover, in case the blood sugar level drops the dashboard unit alarms the driver with an audible warning.
The Future of Diabetes Technology
Although diabetes management might be difficult, there is a bright future with many technologies and studies in development.
Some of them are the robotic pancreas, i.e., closed- a looped pump that monitors the blood glucose levels and delivers insulin in only one unit. Moreover, blood sugar tests with a breathalyzer-style system similar to blood alcohol units.
Glucowizzard and Microsoft
A device in development is the Glucowizzard. This a device that removes the painful pricks. Instead of that, an implant as big as a grain of rice is placed under the skin of a patient.
This implant monitors the blood sugar levels and delivers the info to a solar-powered watch. This device will make life much easier for all who have diabetes. Also, Microsoft is creating a contact lens that can read blood glucose levels.
When it comes to diabetes, the journey is really fascinating.